Most healthcare organisations are investing more in marketing than ever before. Yet, many leadership teams continue to deal with high volumes of patient inquiries and only a limited number of confirmed appointments.
The root cause is rarely found in marketing budgets or promotional channels. More often, it lies in how patient data is captured, managed, and used across the organisation.
In many hospitals, clinics, and diagnostic labs, patient information remains fragmented across multiple platforms and teams. As a result, decision-makers struggle to prioritise leads, ensure timely follow-ups, and accurately measure performance. Without structured data systems, growth becomes dependent on individual effort rather than organisational capability.
This is where data-driven patient acquisition makes a meaningful difference. Data-driven systems that centralise, analyse, and activate patient data enable healthcare organisations to gain greater clarity and control over their growth processes.
This blog explores how hospitals, clinics, and diagnostic labs can apply data-driven approaches in practical, real-world scenarios to increase patient appointments. The focus is not on theoretical models or exaggerated success stories, but on frameworks that can be implemented, measured, and sustained over time.
Understanding Healthcare Data in Marketing & Operations
To understand how data improves patient appointments, it is important to first understand what kind of data healthcare organisations actually work with, and how it connects marketing with daily operations.
Healthcare organisations typically work with multiple categories of data, often spread across different systems and departments.
Key Types of Healthcare Data Include:
Patient Enquiry and Lead Data
This includes information collected through websites, landing pages, call centres, walk-ins, and referrals. It covers details such as name, contact information, enquiry source, service interest, and preferred appointment time.
Marketing Performance Data
This data tracks how patients discover the organisation. It includes campaign performance, website traffic, ad engagement, conversion rates, and cost per lead. It helps teams understand which channels are generating quality inquiries.
Appointment and Scheduling Data
This includes booking status, reschedules, cancellations, no-shows, and waiting lists. It reflects how efficiently patient interest is converted into actual visits.
Clinical and Service Data
This covers department-wise demand, doctor availability, test volumes, and treatment preferences. It helps align marketing efforts with operational capacity.
Communication and Follow-Up Data
This includes call records, SMS reminders, email interactions, and WhatsApp conversations. It shows how consistently and effectively patients are being engaged.
Patient History and Engagement Data
This captures past visits, repeat consultations, test frequency, and loyalty patterns. It is critical for retention and long-term growth.
Individually, each of these data sets provides limited value. However, when they are integrated and analysed together, they create a complete view of the patient journey.
When data is fragmented or incomplete, teams operate reactively; as a result, conversion rates remain inconsistent. In contrast, when patient data is structured and accessible, it enables proactive decision-making.
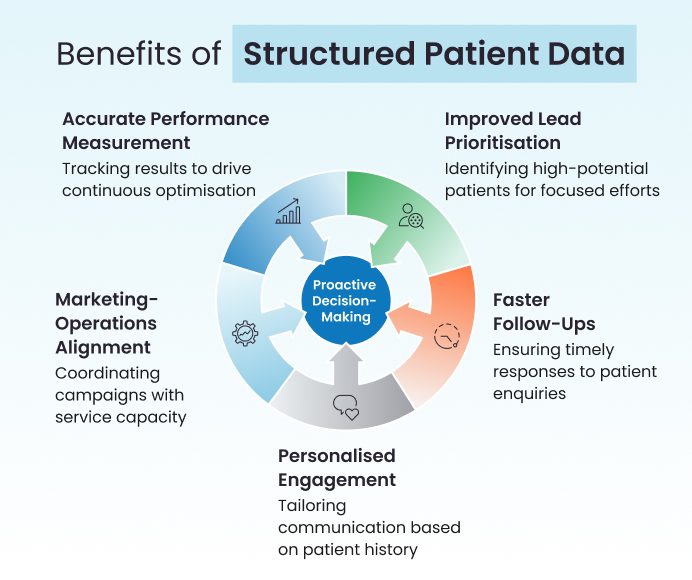
Over time, these improvements compound. What begins as better data management evolves into stronger systems, higher accountability, and predictable appointment growth.
In healthcare, appointment conversion is driven by clarity, coordination, and consistency, all of which are enabled by data.
Common Challenges in Managing Patient Appointments Without Data
In today’s healthcare environment, patient acquisition and appointment management cannot be sustained through intuition, manual tracking, or fragmented systems. As enquiry volumes increase and patient expectations rise, managing growth without structured data becomes increasingly difficult. What may work at a small scale quickly breaks down as operations expand.
While the challenges may appear different across hospitals, clinics, and diagnostic labs, they generally fall into three fundamental areas.
Low Lead Conversion Rates
One of the most visible consequences of poor data management is low enquiry-to-appointment conversion.
When patient information is incomplete, scattered, or outdated, teams struggle to identify which enquiries require immediate attention.
- High-intent patients are treated the same as casual enquiries.
- Follow-ups are not prioritised based on urgency or service need.
As a result, many potential appointments are lost despite strong lead volumes.
In the absence of structured data, teams often rely on memory, personal judgment, or informal notes to manage leads. Data-driven systems solve this by enabling lead scoring, segmentation, and prioritisation. Without these capabilities, improving conversion becomes largely a matter of chance.
Missed Follow-Ups and Delayed Responses
Timely communication plays a critical role in patient decision-making. Delays in response reduce trust, create uncertainty, and increase the likelihood of patients choosing alternative providers.
Without centralised data systems, follow-up responsibilities are often unclear.
- Enquiries may be recorded in different tools, personal devices, or paper registers.
- Team members may assume someone else has responded. Important reminders are missed.
- Callback schedules are not maintained.
Over time, these small lapses accumulate into significant revenue loss.
Delayed responses also affect internal efficiency. Teams spend time searching for information, confirming previous interactions, and resolving communication gaps. Data-enabled workflows, automated reminders, and shared visibility prevent these issues. In their absence, missed follow-ups remain one of the most persistent barriers to appointment growth.
Lack of Visibility Into Marketing Performance
Many healthcare organisations invest in multiple channels. However, without proper data tracking, leadership teams often struggle to determine which initiatives are generating quality appointments and which are merely producing enquiries.
To address these inefficiencies, organisations must first identify the specific disconnects within their reporting frameworks:
- Metrics such as lead volume, conversion rate, cost per appointment, and channel-wise performance remain unclear or unreliable.
- Decisions are made based on surface-level indicators rather than real outcomes.
This lack of visibility leads to inefficient budget allocation. High-performing channels may be underfunded, while low-impact campaigns continue unchecked. When data is structured and integrated, marketing performance becomes transparent and measurable.
Taken together, these challenges reflect a deeper structural issue rather than isolated operational gaps. Addressing these issues requires a structured framework that integrates data into every stage of the patient journey.
Use Case Framework: How Data Improves Patient Appointment Systems
Addressing appointment conversion challenges requires a structured framework that connects marketing, operations, and patient engagement through data. A well-defined use case framework helps healthcare organisations move from reactive management to system-driven growth.
The foundation of this approach rests on four interconnected components.
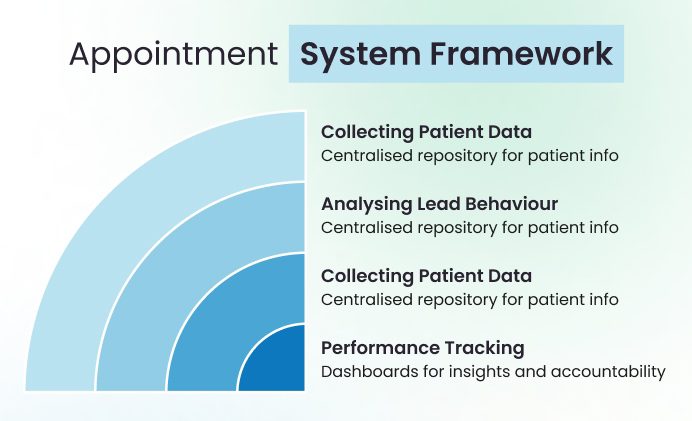
Collecting and Centralising Patient Data
The first step in building an effective appointment system is ensuring that all patient-related data is captured and stored in one central platform.
A centralised data system brings all patient interactions into a single, accessible repository. This creates a unified patient profile that can be accessed by relevant teams in real time. With centralisation, organisations gain consistency, accountability, and continuity. Even when staff members change or workloads increase, patient information remains organised and reliable.
When implemented correctly, this framework improves appointment systems and strengthens organisational capability and scalability.
Analysing Lead Behaviour and Intent
Once data is centralised, the next step is to analyse how patients interact with the organisation and what their behaviour indicates about intent.
Not all enquiries carry the same level of urgency or conversion potential. Some patients are actively seeking immediate appointments, while others are in an early research stage. Without data analysis, these differences remain invisible. By studying engagement patterns, enquiry sources, service interests, response times, and past interactions, teams can identify high-intent leads and prioritise them effectively. This enables smarter allocation of time and resources.
Behavioral analysis also helps leadership understand demand trends, seasonal patterns, and service preferences. These insights support better planning and more targeted marketing strategies.
Automating Follow-Ups and Reminders
Consistent follow-up is one of the most critical factors in appointment conversion. However, manual follow-up systems are difficult to maintain at scale and are highly dependent on individual discipline.
Automation addresses this limitation.
With data-driven workflows, follow-up tasks, reminders, and notifications are triggered automatically based on predefined rules. Teams receive timely prompts for callbacks, confirmations, and rescheduling. Patients receive reminders through appropriate communication channels. This reduces dependency on memory and manual tracking. It ensures that no enquiry is overlooked and that engagement remains consistent across touchpoints.
Automation also improves operational efficiency by reducing administrative workload, allowing staff to focus more on patient interaction and service quality.
Tracking Performance Through Dashboards
The final component of the framework is performance tracking through integrated dashboards.
Dashboards transform raw data into actionable insights. They provide leadership teams with real-time visibility into key metrics such as enquiry volume, conversion rates, response times, appointment confirmations, and channel performance. With access to accurate dashboards, decision-makers can identify bottlenecks, evaluate team productivity, and assess return on marketing investments.
Performance tracking also promotes accountability and continuous improvement. Teams understand how their efforts contribute to outcomes, and optimisation becomes part of routine operations.
When used consistently, dashboards shift organisational culture from opinion-based decision-making to evidence-based management.
Use Case 1: How Hospitals Use Data to Optimise Appointment Scheduling
Hospitals handle a high volume of patient inquiries across multiple departments every day. Managing these appointments efficiently is critical for patient experience, clinical outcomes, and revenue performance.
Without data-driven systems, scheduling often depends on manual coordination and incomplete information. By applying structured data frameworks, hospitals can bring clarity, predictability, and efficiency to appointment management.
Identifying High-Intent Patients
Data analysis helps hospitals identify high-intent patients based on enquiry sources, service requirements, and engagement behaviour. These patients can be prioritised for faster responses and suitable time slots. This focused approach improves conversion rates and ensures that critical cases receive timely care.
Reducing No-Shows and Drop-Offs
No-shows and cancellations lead to wasted capacity and operational inefficiencies. With structured data, hospitals can identify patterns related to missed appointments and deploy automated reminders, confirmations, and rescheduling options. Personalised communication further strengthens patient commitment.
Over time, these measures improve attendance rates and schedule reliability.
Improving Department-Wise Conversions
Each hospital department has unique demand and performance patterns. Data-driven analysis enables leadership teams to track department-wise enquiries, bookings, and outcomes. This supports better resource allocation, targeted marketing, and operational optimisation.
By using data to prioritise patients, reduce drop-offs, and optimise departmental performance, hospitals can transform appointment scheduling into a strategic growth function.
Use Case 2: How Clinics Use Data to Increase Patient Retention
For clinics, long-term growth depends not only on attracting new patients but also on building strong relationships with existing ones. However, many clinics focus heavily on acquisition while overlooking structured retention systems.
By using data strategically, clinics can create personalised, reliable, and patient-centric engagement models that encourage repeat visits and sustained trust.
Personalised Communication Strategies
Patients are more likely to return when communication feels relevant and timely. Data enables clinics to personalise interactions based on medical history, appointment patterns, preferences, and previous conversations. Reminders can be tailored to specific services, follow-ups can reference past visits, and health updates can be aligned with individual needs.
This personalized approach improves patient satisfaction and strengthens emotional connection with the clinic, increasing the likelihood of continued engagement.
Repeat Visit and Loyalty Tracking
Data systems help monitor visit frequency, treatment cycles, test intervals, and referral patterns. This makes it easier to identify loyal patients, high-value segments, and disengagement risks. With these insights, clinics can design targeted loyalty programmes, preventive care reminders, and re-engagement campaigns that support long-term relationships.
Consistent tracking transforms retention from a passive outcome into an active growth strategy.
Improving Doctor Availability Planning
Doctor availability plays a critical role in patient retention. Data analysis helps clinics understand peak demand periods, preferred consultation timings, and doctor-specific booking trends. This supports better schedule planning and workload distribution.
By aligning doctor availability with patient demand, clinics can reduce waiting times, improve appointment access, and enhance overall service experience.
Use Case 3: How Diagnostic Labs Use Data to Boost Test Bookings
Diagnostic labs operate in a highly competitive environment where efficiency, accessibility, and service relevance directly influence patient choice. Without structured data systems, test bookings are driven largely by seasonal trends, walk-ins, and fragmented referrals. This makes revenue unpredictable and limits long-term planning.
By applying data-driven frameworks, diagnostic labs can gain deeper visibility into patient behaviour, service demand, and market opportunities, enabling more consistent and scalable growth.
Analysing Test Demand Patterns
Different diagnostic tests experience varying levels of demand based on seasonality, demographics, lifestyle trends, and public health factors. Data analysis helps labs track test-wise volumes, frequency patterns, and peak periods. This enables better inventory planning, staffing allocation, and equipment utilisation.
By understanding which tests are in high demand and when, labs can also design targeted promotions and awareness campaigns, improving booking consistency throughout the year.
Location-Based and Service-Based Insights
Patient preferences often vary significantly based on location, accessibility, and service availability. Data allows labs to analyse booking trends across branches, collection centres, and home sample services. It highlights which locations perform well, which require operational improvement, and where expansion opportunities exist.
Service-based insights further reveal which test categories drive maximum revenue and engagement. This supports better service positioning and targeted outreach strategies.
Cross-Selling and Upselling Through Data
Diagnostic labs generate significant growth opportunities through bundled tests, preventive health packages, and follow-up diagnostics. Data-driven systems help identify patients who may benefit from additional tests based on medical history, previous reports, age, or risk factors. This enables personalized recommendations that are relevant and clinically appropriate.
Cross-selling and upselling become value-driven rather than promotional, improving patient trust while increasing average booking value.
By leveraging demand analysis, location insights, and personalised recommendations, diagnostic labs can use data to strengthen booking volumes and revenue stability.
Step-by-Step Process: Implementing a Data-Driven Appointment System
Moving to a data-driven appointment system requires a structured implementation approach that aligns technology, processes, and people. Successful healthcare organisations treat data transformation as a phased journey rather than a one-time project.
The visual framework below summarises this implementation process and highlights how data flows from assessment to execution and optimisation.
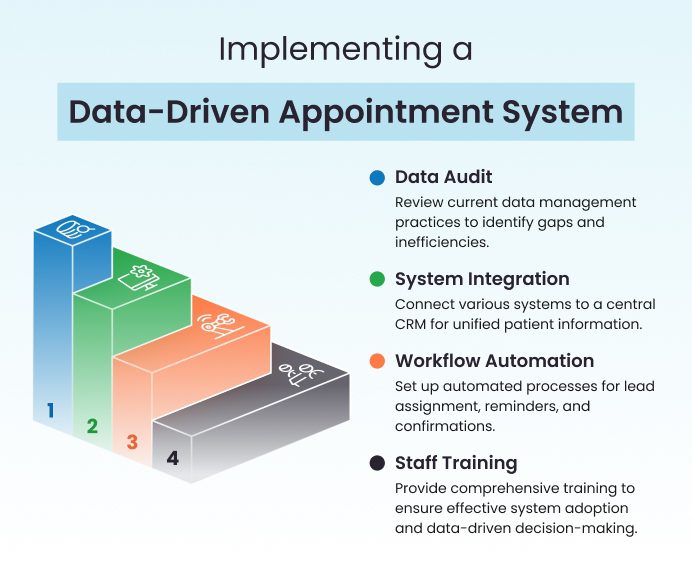
Data Audit and Gap Analysis
This involves reviewing how patient information is collected, stored, shared, and used across departments. Leadership teams must identify data sources, duplication issues, missing records, and manual dependencies.
A structured audit reveals operational gaps, process inefficiencies, and compliance risks. It also clarifies which systems require improvement and which practices need standardisation.
CRM and System Integration
This typically involves connecting websites, call systems, appointment tools, messaging platforms, and internal databases with a central CRM or management system. Integration ensures that all patient interactions are captured in real time and remain accessible to relevant teams. A unified system eliminates silos, reduces duplication, and improves coordination between marketing, operations, and clinical staff.
Workflow Automation Setup
After centralisation, workflows must be designed to ensure consistent execution. This includes setting up automated lead assignment, follow-up reminders, appointment confirmations, rescheduling alerts, and escalation triggers. These workflows are based on predefined rules and patient behaviour patterns.
Automation reduces dependency on manual tracking and minimises human error. It ensures that every enquiry follows a structured journey from first contact to confirmed appointment.
Staff Training and Adoption
Technology and processes deliver value only when teams understand and adopt them effectively. Comprehensive training is essential to ensure that staff members know how to use systems correctly, interpret data insights, and follow standard workflows. Training should focus not only on functionality but also on the business impact of data-driven practices.
Ongoing support, performance reviews, and feedback mechanisms further strengthen system utilisation and long-term success.
By following this structured implementation process, healthcare organisations can transition smoothly from fragmented operations to integrated, data-driven appointment systems. The result is stronger execution, higher accountability, and sustainable performance improvement.
Key Benefits of Using Data for Patient Appointment Growth
Implementing a data-driven appointment system delivers measurable value across marketing, operations, and patient engagement. Beyond improving daily workflows, it strengthens organisational performance and supports long-term sustainability.
When data is used consistently and strategically, healthcare organisations move from reactive problem-solving to proactive growth management. The benefits extend beyond short-term gains and contribute to lasting competitive advantage.
- Higher Conversion Rates: By prioritising high-intent leads, enabling timely follow-ups, and personalising communication, organisations significantly reduce lead leakage. With clear visibility into the patient journey, gaps can be identified and corrected quickly. Over time, this results in more consistent and predictable conversion performance.
- Lower Patient Acquisition Cost: Data enables leadership teams to identify high-performing channels, eliminate inefficient campaigns, and optimise budget allocation. Resources are directed towards strategies that deliver confirmed appointments rather than just enquiries. Improved conversion rates also reduce dependency on continuous lead generation, lowering the overall cost of acquiring each patient.
- Better Patient Experience: Data-driven systems enable faster responses, personalised interactions, and seamless appointment management. Patients receive timely reminders, clear information, and consistent support throughout their journey. Reduced waiting times, fewer scheduling errors, and smoother follow-ups strengthen patient trust and satisfaction.
- Scalable Growth Systems: Data-driven systems create standardised, repeatable processes that can support higher enquiry volumes without proportional increases in staff or complexity. These systems also reduce dependency on specific individuals, ensuring continuity during team transitions and periods of high demand.
Organisations that invest in structured data systems position themselves for long-term success in an increasingly competitive healthcare environment.
Best Practices for Healthcare Organisations Using Patient Data
As healthcare organisations increasingly rely on data for growth and decision-making, it becomes essential to follow structured best practices. Leading healthcare agencies and growth teams focus on building systems that balance performance, security, and compliance.
Below are the key best practices for managing patient data effectively.
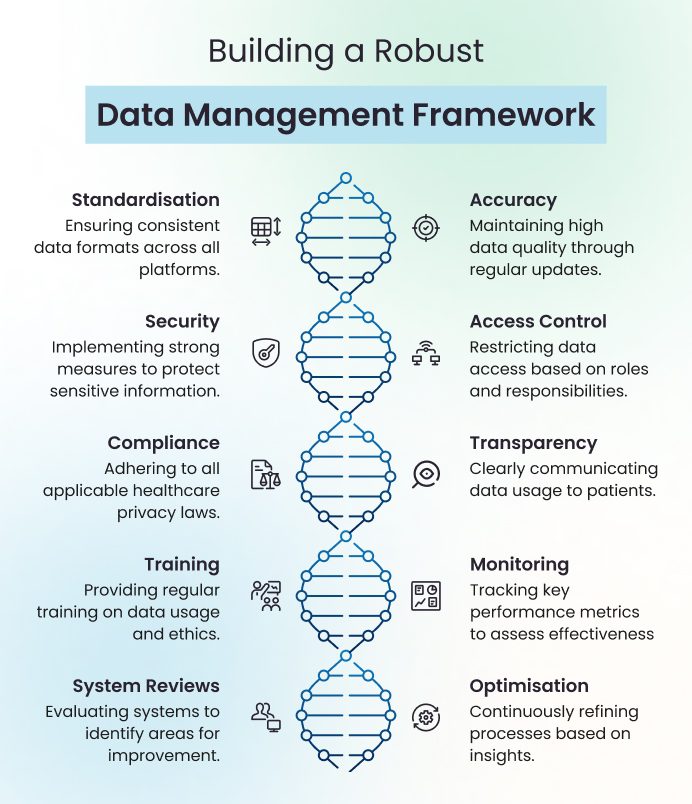
By consistently following these best practices, healthcare organisations can transform patient data into a reliable strategic asset. When managed responsibly, data becomes a foundation for sustainable, compliant, and performance-driven healthcare delivery.
Conclusion
Sustainable patient appointment growth is built on structured data systems that connect marketing, operations, and patient engagement into one cohesive framework.
Hospitals, clinics, and diagnostic labs that invest in data-driven processes gain clarity, consistency, and control over their growth journey. Organisations that act early and implement structured frameworks today will be better positioned to lead tomorrow.
If your organisation is struggling with low conversion rates, missed follow-ups, unclear performance metrics, or inconsistent growth, it may be time to adopt a more structured, data-led approach. MedGrowthEngine.ai helps healthcare organisations design, implement, and optimize end-to-end patient acquisition and appointment systems. Our team combines industry expertise, advanced analytics, and automation-driven workflows to create measurable and sustainable growth models.
Schedule a free growth audit or strategy consultation to understand how data-driven systems can transform your patient acquisition process.







