In a highly competitive healthcare environment, the real challenge lies in converting enquiries into confirmed appointments and long-term patient relationships. While digital marketing has increased visibility, it has also exposed critical gaps in how healthcare organisations manage and nurture patient intent.
Rising acquisition costs, increasing patient expectations, and fragmented internal systems have made conversion optimization a strategic priority. Delayed responses, inconsistent follow-ups, and limited visibility across teams directly impact revenue and brand credibility.
For marketing heads, practice managers, and growth leaders, conversion efficiency, along with performance indicators such as traffic and lead volume, matters the most, as these directly reflect how effectively patient interest is translated into business outcomes.
As a result, successful healthcare organisations focus on attracting patients and also building structured, technology-driven systems that maximise every opportunity. By improving enquiry handling, follow-up processes, and appointment management, they create predictable and scalable growth.
To understand how these challenges emerge, it is essential to examine the current state of healthcare lead management and patient engagement practices.
The Current State of Healthcare Lead Management
Despite increased investments in digital marketing and patient acquisition, many healthcare organisations continue to operate with fragmented lead management systems. This creates data silos, which in turn prevent teams from gaining a complete view of the patient journey, resulting in inconsistent engagement and missed opportunities.
In the absence of integrated systems, most follow-up processes remain heavily manual. This leads to delayed responses, irregular communication, and dependency on individual availability. As a result, healthcare organisations commonly face the following operational challenges:
- Disconnected lead sources with no central visibility
- Manual data entry and inconsistent record management
- Delayed or missed follow-ups
- Lack of standardised engagement workflows
- Limited performance tracking and reporting
These challenges create hidden revenue leakage points throughout the patient acquisition funnel. Over time, these inefficiencies accumulate into substantial financial losses, often without being clearly reflected in standard performance reports.
Furthermore, limited visibility into lead movement and patient engagement makes it difficult for leadership teams to identify bottlenecks or optimize processes. Without accurate, real-time data, decision-makers are forced to rely on assumptions rather than actionable insights, weakening both marketing effectiveness and operational planning.
Collectively, fragmented systems, manual processes, and invisible revenue losses undermine growth potential. Addressing these challenges requires a deeper understanding of how patients move through the acquisition and conversion journey.
Understanding the Patient Acquisition and Conversion Funnel
Every patient relationship begins long before the first consultation and continues well beyond the initial appointment. Yet, many healthcare organisations focus only on isolated stages of this journey, rather than managing it as a connected system.
At the centre of sustainable healthcare growth lies a clearly defined patient acquisition and conversion funnel. It is a framework that maps how prospective patients progress through each decision-making stage. When managed effectively, this funnel enables organisations to align marketing, operations, and clinical teams around shared performance outcomes.
A typical healthcare conversion funnel follows this structured path: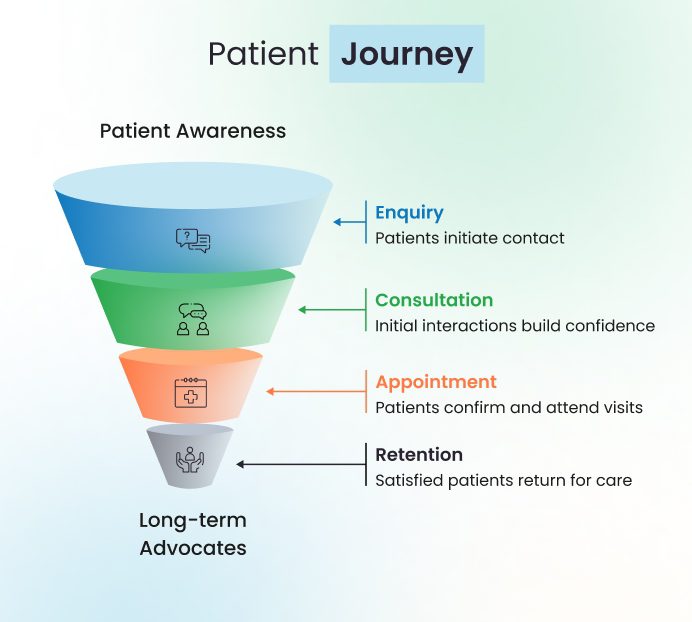
This funnel can be visualised as a narrowing pathway, where each stage filters patient intent based on experience, responsiveness, and perceived value.
However, most healthcare organisations experience significant patient drop-offs at critical transition points. Some of the common loss areas include:
- Delayed enquiry responses
- Inconsistent consultation follow-ups
- Unclear appointment scheduling processes
- And a lack of post-visit engagement.
Although industry observations indicate that the largest conversion declines typically occur between enquiry and consultation, as well as between consultation and confirmed appointments. These gaps weaken trust and often push patients toward more responsive competitors.
To manage this effectively, leadership teams must monitor key conversion benchmarks across each stage, including enquiry-to-consultation rate, consultation-to-appointment rate, show-up rate, and repeat-visit percentage. These indicators provide clear visibility into funnel health and highlight where corrective action is required.
To strengthen funnel outcomes, it is therefore essential to identify the key operational and strategic barriers that limit patient progression at each stage.
Key Challenges Impacting Enquiries and Conversions
While many healthcare organisations invest significantly in patient acquisition, few achieve consistent and predictable conversion outcomes. This gap results from structural and operational challenges that weaken the connection between marketing efforts and patient engagement.
Some of the most critical challenges impacting enquiries and conversions include:
- Poor Lead Qualification: Not all enquiries represent genuine patient intent. Without structured qualification criteria, teams often treat every lead equally, resulting in wasted time and misallocated resources. High-potential prospects may receive insufficient attention, while low-intent leads consume operational capacity, reducing overall conversion efficiency.
- High Cost per Acquisition (CAC): Rising competition and increasing digital advertising costs have significantly inflated patient acquisition expenses. When conversion systems are weak, organisations are forced to spend more to generate the same number of confirmed appointments. This imbalance directly affects profitability and limits long-term scalability.
- Inconsistent Follow-Up Processes: In many organisations, follow-ups depend heavily on individual staff members rather than standardised workflows. This leads to irregular communication, missed touchpoints, and variable patient experiences. Inconsistent engagement weakens trust and reduces the likelihood of appointment confirmation.
- Low Lifetime Patient Value: A narrow focus on first-time conversions often overshadows long-term relationship building. Limited post-visit engagement, lack of continuity in care communication, and absence of retention strategies result in low repeat visits and weak patient loyalty. Over time, this reduces the overall return on marketing and operational investments.
Collectively, these challenges create systemic inefficiencies that restrict growth and increase financial risk. Addressing them requires more than isolated improvements; it demands integrated systems, data-driven decision-making, and process automation.
To overcome these barriers effectively, healthcare leaders must leverage the strategic role of technology, analytics, and intelligent automation in driving conversion performance.
The Role of CRM, SEO, Automation, and AI in Healthcare Growth
As healthcare organisations scale their marketing and patient acquisition efforts, traditional systems increasingly struggle to keep pace. Legacy approaches restrict visibility, delay decision-making, and prevent leadership teams from responding proactively to market dynamics.
In today’s competitive environment, sustainable growth depends on the intelligent integration of three critical capabilities:
- Structured data management
- Consistent digital visibility
- Advanced performance intelligence
CRM, SEO, and AI-driven analytics have therefore become essential components of modern healthcare growth strategies. Together, they enable organisations to manage patient relationships systematically, attract high-intent prospects, and optimise conversion processes with precision.
CRM to Improve Visibility
A robust healthcare CRM system serves as the central nervous system of patient engagement. It consolidates enquiries from all channels into a single platform, enabling teams to track every interaction across the patient journey. With real-time access to lead status, follow-up history, and conversion metrics, leadership teams gain complete operational visibility. This transparency supports better accountability, faster response times, and more consistent patient experiences.
SEO as a Long-Term Patient Acquisition Engine
Search engine optimization plays a strategic role in building sustainable patient pipelines. Unlike paid campaigns that stop generating leads once budgets are exhausted, SEO creates continuous digital visibility for high-intent searches related to treatments, services, and locations. By ranking for relevant healthcare queries, organisations attract patients who are actively seeking care, improving lead quality and reducing long-term acquisition costs.
AI-Powered Analytics for Smarter Decisions
AI-driven analytics transform raw data into actionable insights. By analysing enquiry patterns, engagement behaviour, and conversion trends, AI systems identify performance gaps and growth opportunities that may not be visible through manual reporting. Predictive models enable teams to prioritise high-value leads, optimise follow-up timing, and forecast revenue outcomes with greater accuracy.
When CRM, SEO, automation, and AI analytics operate as an integrated ecosystem, healthcare organisations gain the ability to manage growth systematically rather than reactively. To translate these technological capabilities into measurable outcomes, organisations must apply them through a structured, step-by-step conversion improvement framework.
Step-by-Step Model to Improve Patient Enquiries and Conversions
Improving patient enquiries and conversion outcomes requires a structured, repeatable model that aligns marketing, operations, and technology around clearly defined performance objectives.
This step-by-step model outlines how healthcare organisations can systematically strengthen each stage of the patient journey and transform fragmented efforts into scalable growth systems.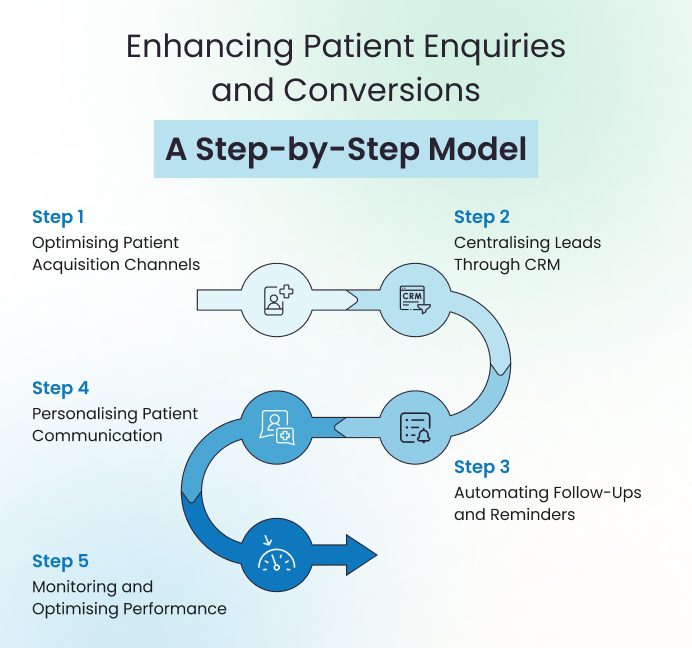
Step 1: Optimising Patient Acquisition Channels
Effective conversion begins with the quality of incoming enquiries. Organisations must evaluate and refine all acquisition channels, including websites, search engines, social platforms, referrals, and partner networks, to ensure they attract high-intent prospects. This involves improving landing page relevance, aligning messaging with patient needs, and continuously testing channel performance. Strong acquisition foundations reduce downstream inefficiencies and improve overall conversion potential.
Step 2: Centralising Leads Through CRM
Once enquiries are generated, centralisation becomes critical. All patient interactions must flow into a unified CRM system to ensure consistent tracking and accountability. Centralised lead management eliminates data silos, reduces duplication, and enables teams to manage follow-ups systematically. This visibility ensures that no enquiry is overlooked and that every prospect receives timely attention.
Step 3: Automating Follow-Ups and Reminders
Manual engagement processes cannot support high-volume, time-sensitive environments. Automation enables organisations to deploy predefined follow-up sequences, appointment reminders, and re-engagement messages across multiple channels. These workflows ensure consistent communication, minimise response delays, and reduce dependency on individual staff availability, significantly improving conversion reliability.
Step 4: Personalising Patient Communication
While automation improves efficiency, personalisation strengthens trust. Patients expect interactions that reflect their specific needs, preferences, and medical interests. By leveraging CRM and behavioural data, organisations can tailor messaging, consultation recommendations, and appointment reminders. Personalised engagement enhances patient confidence and increases the likelihood of long-term retention.
Step 5: Monitoring and Optimising Performance
Sustainable improvement requires continuous measurement and refinement. Leadership teams must regularly review conversion metrics, engagement patterns, and operational bottlenecks. Data-driven optimization enables organisations to adjust acquisition strategies, refine workflows, and improve resource allocation. This ongoing process ensures that performance gains are maintained over time.
When implemented collectively, these five steps establish a disciplined approach to managing patient enquiries and conversions. Rather than relying on reactive problem-solving, organisations gain a structured pathway for predictable growth.
To evaluate the effectiveness of this model, healthcare leaders must track the right performance indicators and benchmarks that directly reflect revenue impact.
Measuring Performance: KPIs That Drive Revenue Growth
In healthcare marketing and operations, improvement is only possible when performance is consistently measured and evaluated. Without clearly defined KPIs, leadership teams lack visibility into what is working, what is underperforming, and where corrective action is required. Tracking the right metrics enables organisations to move from intuition-based decisions to data-driven management, ensuring that growth initiatives deliver measurable financial impact.
Among the various metrics available, the following KPIs play a critical role in driving sustainable growth:
- Lead Response Time: This metric measures how quickly teams respond to new patient enquiries. Faster response times significantly increase the likelihood of engagement and appointment confirmation. Delayed responses, even by a few hours, often result in lost opportunities and reduced patient confidence.
- Appointment Booking Rate: The appointment booking rate reflects the percentage of enquiries that convert into scheduled consultations. It indicates how effectively teams communicate value, address concerns, and guide prospects toward commitment. Low booking rates often signal weaknesses in qualification, follow-up, or consultation processes.
- Show-Up Rate: The show-up rate measures how many scheduled patients actually attend their appointments. Missed visits represent direct revenue loss and operational inefficiency. Automated reminders, clear instructions, and proactive engagement play a key role in improving this metric.
- Conversion Rate: Conversion rate evaluates how many prospects complete desired actions, such as confirming appointments, undergoing procedures, or enrolling in treatment plans. It provides a comprehensive view of funnel performance and reflects the combined impact of marketing, communication, and service quality.
- Retention Rate: Retention rate indicates the percentage of patients who return for continued care. High retention reflects strong patient satisfaction, effective post-visit engagement, and long-term relationship management. Improving this metric significantly increases lifetime patient value and reduces dependency on constant acquisition.
When monitored collectively, these KPIs provide a holistic view of revenue performance and operational effectiveness. They enable leadership teams to diagnose weaknesses early, validate strategic investments, and reinforce high-performing practices.
To maximise the financial impact of KPI-driven management, organisations must also focus on reducing acquisition costs and strengthening return on investment through intelligent systems and optimisation strategies.
Reducing CAC and Improving ROI Through Smart Systems
Cost per Acquisition (CAC) represents the total investment required to acquire a new patient, including marketing spend, operational costs, and engagement resources.
Today, CAC continues to rise due to increasing advertising expenses, intensified competition, and higher patient expectations. When acquisition costs grow faster than conversion and retention rates, profitability and scalability are directly impacted. By strengthening lead quality, streamlining engagement processes, and leveraging data-driven systems, healthcare organisations can generate higher returns from the same or lower investment levels.
Several strategic approaches enable organisations to lower CAC while improving overall ROI.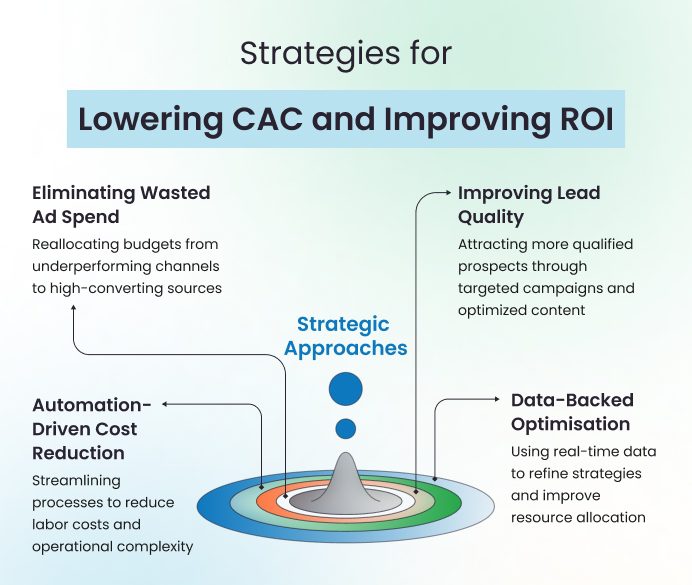
Eliminating Wasted Ad Spend
A significant portion of marketing budgets is often consumed by underperforming channels, poorly targeted campaigns, or irrelevant keywords. Without accurate attribution and performance tracking, these inefficiencies remain hidden.
Smart systems enable teams to identify low-return activities and reallocate budgets toward high-converting sources, ensuring optimal utilisation of marketing resources.
Improving Lead Quality
High enquiry volumes do not necessarily translate into high revenue. By refining audience targeting, optimising landing pages, and aligning content with patient intent, organisations can attract more qualified prospects. Better lead quality reduces time spent on low-intent enquiries and increases the probability of successful conversions.
Automation-Driven Cost Reduction
Manual follow-ups, appointment scheduling, and record management increase labour costs and operational complexity. Automation streamlines these processes through predefined workflows, reminders, and engagement sequences. This reduces administrative burden, minimises errors, and enables teams to manage larger enquiry volumes without proportional cost increases.
Data-Backed Optimisation
Continuous performance improvement requires reliable data insights. Advanced analytics platforms track channel effectiveness, engagement behaviour, and conversion trends in real time. By analysing this data, leadership teams can optimise campaign strategies, refine operational processes, and improve allocation decisions.
When these approaches are implemented collectively, healthcare organisations achieve greater cost efficiency and stronger revenue predictability. Furthermore, to quantify these performance improvements, leaders must adopt structured ROI frameworks that clearly link operational enhancements to financial outcomes.
How to Calculate the Financial Impact of Better Conversions
Understanding the financial impact of improved patient conversions begins with a clear and consistent ROI measurement framework. At its core, healthcare ROI evaluates how effectively marketing and operational investments translate into revenue outcomes.
A simple and widely applicable formula is:

Alongside this, leadership teams should closely monitor key performance indicators such as conversion rate, average revenue per patient, Cost per Acquisition (CAC), and retention rate. Together, these metrics provide a reliable foundation for evaluating financial performance across the patient journey.
One of the most immediate benefits of conversion optimization is revenue uplift. Even modest improvements in enquiry-to-appointment or consultation-to-confirmation rates can generate significant financial gains.
For example: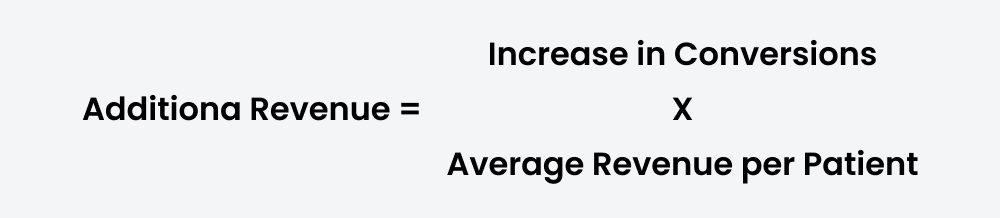 If an organisation converts 50 additional patients per month at an average value of ₹20,000 per patient, the resulting monthly revenue uplift is ₹10,00,000. Such improvements compound over time, creating sustained growth without proportional increases in marketing spend.
If an organisation converts 50 additional patients per month at an average value of ₹20,000 per patient, the resulting monthly revenue uplift is ₹10,00,000. Such improvements compound over time, creating sustained growth without proportional increases in marketing spend.
Automation further strengthens financial performance by reducing operational costs. Automated follow-ups, appointment reminders, lead routing, and reporting minimise manual workload and staffing dependencies. This leads to lower administrative expenses, fewer errors, and improved productivity.
Cost savings from automation can be calculated as: When combined with improved conversion rates, these savings directly enhance profit margins and capital efficiency.
When combined with improved conversion rates, these savings directly enhance profit margins and capital efficiency.
Beyond immediate revenue and cost benefits, long-term financial impact is driven by patient retention. Retained patients generate recurring revenue through follow-up consultations, procedures, and referrals. They also require lower acquisition investment compared to new prospects.
The long-term value of patient relationships can be assessed through:

Higher retention rates significantly increase LTV, stabilise cash flows, and reduce dependency on continuous acquisition campaigns.
To support these financial gains at scale, organisations must build a robust infrastructure that aligns technology, processes, and people around sustainable growth objectives.
Conclusion
This guide has highlighted that sustainable healthcare growth is driven not by the volume of enquiries but by the ability to convert, engage, and retain patients effectively. By addressing fragmented systems, strengthening follow-ups, leveraging CRM, SEO, automation, and AI, and tracking the right KPIs, organisations can build predictable and scalable growth models.
Adopting a future-ready growth mindset is now essential. Conversion excellence has become a strategic differentiator that directly impacts profitability, brand credibility, and patient satisfaction. Organisations that prioritise structured processes and data-driven decision-making are better positioned for long-term success.
To accelerate this transformation, healthcare leaders should begin with a Comprehensive Growth Audit. An audit provides clear visibility into acquisition efficiency, conversion performance, operational gaps, and revenue leakage points. It enables decision-makers to identify improvement opportunities and develop targeted optimisation strategies.
By requesting a growth audit, leaders gain actionable insights, performance benchmarks, and a practical roadmap for improving ROI and patient lifetime value. Start your growth audit today, or contact the sales team to explore how MedGrowthEngine.ai can support your growth objectives.







