Most hospitals don’t really have an “ads problem.” They have a data visibility problem. I’ve seen hospitals with strong reputations, skilled doctors, functional websites, and steady advertising budgets, yet leadership teams still ask the same question in review meetings: “Why are patient enquiries not increasing?”
Despite consistent marketing investments, expected growth often fails to materialise.
The truth is, enquiries don’t always decline because marketing performance gets worse. More often, they decline because leads are leaking silently through parts of the system that are not being tracked properly, not being qualified consistently, or not being followed up on fast enough. When important data is missing and processes are unclear, small gaps gradually turn into lost opportunities.
This is why one principle guides everything we do: AI and automation only work when your tracking and follow-up system is clean. If the system is disorganised, automation doesn’t fix it. It simply amplifies the problem.
Let me start with a painfully common story.
A Common Hospital Scenario: High Lead Volume, Low Usability
A mid-size multi-specialty hospital in Ahmedabad was generating a steady stream of enquiries through WhatsApp and website forms. On paper, everything looked active. Campaigns were running, the marketing team was reporting healthy lead numbers, and management was investing consistently in promotions.
Yet, on the ground, the front desk team was frustrated.
Many callers were only enquiring about prices. Some were located outside the hospital’s service area. Others were not even looking for the hospital’s core specialties. Despite spending hours responding to enquiries, OPD bookings were not improving in proportion to the reported lead volume.
The problem was not the number of leads.
It was the quality of those leads and the lack of clarity in how they were being tracked and evaluated. Every enquiry was being counted as a success, regardless of intent, relevance, or conversion potential. Qualified patient enquiries were not being separated from casual or unsuitable enquiries.
As a result, leadership saw “activity,” while operations experienced stagnation.
This is where many hospitals unknowingly lose momentum. Good ads create visibility and engagement. Clean, structured data creates outcomes.
What We Mean by “Patient Enquiry”?
In this article, when I refer to a patient enquiry, I am referring to high-intent actions that indicate genuine interest in seeking care.
These include:
- Direct phone calls
- Meaningful WhatsApp conversations with clear treatment intent
- Confirmed appointment bookings.
These are fundamentally different from low-intent actions such as page views, clicks, or time spent on a website. While such metrics can serve as useful signals of engagement, they are not outcomes. On their own, they do not reflect real patient acquisition or revenue potential.
For sustainable growth, every hospital system must be able to answer one critical question with clarity and consistency:
Which marketing efforts are generating qualified calls, intent-driven conversations, and confirmed bookings versus those that ensure only surface-level activity?
When this distinction is unclear, marketing budgets are often misallocated, operational teams become frustrated, performance reviews turn unproductive, and accountability becomes blurred. Over time, growth becomes inconsistent and increasingly difficult to predict.
Two Operational Realities Behind Enquiry Leakage
Even with well-designed campaigns and consistent marketing activity, many hospitals continue to lose potential enquiries due to a few recurring operational blind spots. These issues are rarely visible in standard reports, but they directly affect conversion outcomes.
Let’s have a look at them:
Speed
Today’s patients rarely contact just one provider. They compare options, enquire simultaneously, and expect quick, professional responses. When follow-ups are delayed, the intent window closes quickly. By the time a response is sent, the patient has often already moved on.
Clarity
When calls, WhatsApp conversations, and form enquiries are not tracked accurately across channels, leadership loses visibility into what is truly driving results. High-performing campaigns appear average, underperforming initiatives seem active, and budget decisions are made on incomplete information. Over time, resources are shifted away from what works and invested further into what does not.
Together, slow response systems and weak attribution structures create silent but significant enquiry leakage.
This is why light performance indicators and surface-level dashboards are not enough. Hospitals need disciplined systems that connect marketing activity to real patient outcomes.
With that context, let us now move into the framework.
The Five Data Blind Spots That Reduce Patient Enquiries
One of the biggest risks in hospital marketing today is false confidence.
When leadership teams rely on incomplete or fragmented data, decisions are made with partial visibility. Over time, this creates a growing gap between perceived performance and actual outcomes.
These blind spots are rarely the result of negligence. They emerge gradually as systems expand, platforms multiply, and processes evolve without consistent governance.
The following five blind spots represent the most common sources of this hidden risk.
Blind Spot #1: The Lead Quality Blind Spot
Many hospitals focus heavily on lead volume. Reports show rising enquiry numbers, yet on the ground, front desk teams remain dissatisfied, and leadership gradually begins to question the real impact of these results.
This gap exists because not all leads reflect genuine patient intent.
A lead becomes a qualified enquiry only when it shows:
- Clear specialty relevance
- Practical location feasibility
- Alignment with available services
- A realistic treatment timeline
- A genuine intent to proceed.
Without these elements, enquiries consume operational time without contributing meaningfully to growth.
When every enquiry is counted as a success, performance metrics look encouraging, but hospital outcomes remain stagnant. Over time, this weakens internal trust and makes growth difficult to sustain.
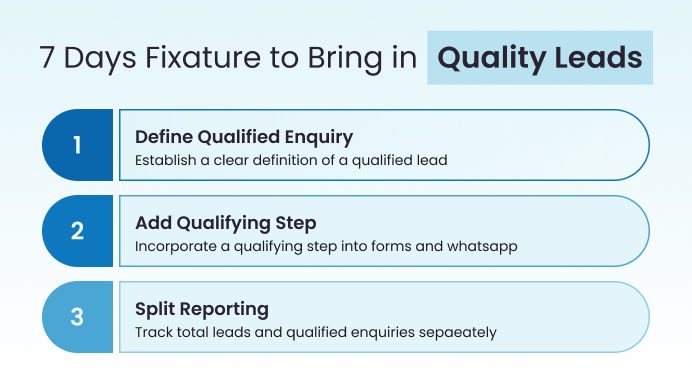
This is why improving lead quality is not a long-term transformation project. With focused alignment and simple process corrections, most hospitals can eliminate this blind spot within days.
To correct this blind spot, we have outlined a practical 7-day improvement plan.
Blind Spot #2: The Source Attribution Blind Spot
Many hospitals invest across multiple digital channels, including Google Search, local listings, social media, SEO, and WhatsApp campaigns. Yet, the leadership team wonders about what channels are actually generating patient calls and serious treatment-related enquiries.
This is one of the most expensive blind spots in hospital marketing.
When calls and high-intent WhatsApp conversations are not tracked accurately, marketing teams are forced to optimise what they can measure most easily, rather than what truly drives revenue. As a result, budget decisions become distorted, high-performing channels are underfunded, and low-impact sources receive continued investment.
Over time, this weakens return on investment and erodes leadership confidence in performance reporting.
To correct this gap quickly, a focused 7-day action plan is outlined below.
![]()
Blind Spot #3: The Intent Alignment Blind Spot
Many hospitals rely on broad, generic messaging such as “Best hospital in Ahmedabad,” “Advanced care,” or “Book an appointment now.” While these messages create visibility, they assume that all patients think, decide, and act in the same way.
In reality, patients are not a single audience. Patient’s concerns, urgency levels, and decision criteria vary significantly. Even within the same specialty, patient intent evolves across stages, ranging from first-time enquiries seeking information, to comparison-driven prospects evaluating options, to patients who are ready to book and expect immediate responses.
When campaigns, landing pages, and follow-up systems treat all these segments identically, relevance is lost. Engagement may continue, and leads may still come in, but conversion quality remains inconsistent. Over time, this misalignment between patient intent and communication strategy weakens trust, reduces responsiveness, and limits sustainable growth.
To address this gap, a focused 7-day action plan is outlined below.

Most hospitals do not need higher marketing spend. They need clearer visibility into what is working, what is leaking, and where growth is being constrained.
To support this, we have developed the Healthcare Marketing Growth Audit.
The audit provides:
- A concise score of your data visibility and funnel health
- Clear identification of the key leakage points affecting patient enquiries
- Three practical, prioritised recommendations that are actionable, not generic
For organisations seeking deeper clarity, a follow-up discussion can also be requested. Our team will review the findings and outline relevant next steps based on your operational context.
Blind Spot #4: The Response-Time Blind Spot
Hospitals often underestimate how much revenue is lost in the first 5 to 30 minutes after an enquiry is received. During this brief window, patient intent is highest and so is competition.
Most patients contact multiple providers within minutes. The first hospital to respond with clarity and relevance usually secures the enquiry. Delayed responses are quickly perceived as disinterested, regardless of clinical quality or reputation.
When follow-ups rely mainly on manual effort, delays become inevitable. WhatsApp messages are missed, callbacks are postponed, leads remain unassigned, and front-desk teams become overloaded—especially after hours. Over time, these gaps create silent but significant enquiry leakage.
To correct this quickly, a focused 7-day action plan is outlined below.

Blind Spot #5: The Outcome Alignment Blind Spot
Many hospitals closely track marketing metrics such as impressions, clicks, leads, and cost per lead. While these figures indicate activity, they do not reflect real business performance.
What truly matters is often measured inconsistently.
Appointments booked, OPD visits, consultation conversions, and patient retention touchpoints determine revenue and long-term growth. When marketing efforts are not connected to these outcomes, visibility is lost, leadership confidence weakens, and budget decisions become subjective.
The objective is not to generate more leads, but to convert qualified enquiries into consistent, booked appointments and sustainable patient relationships.
To correct this gap quickly, a focused 7-day action plan is outlined below.
![]()
What I’m Seeing Across Hospitals in 2026: A Leadership Perspective
Across hospitals and multi-specialty clinics, consistent growth is driven by operational discipline and system maturity.
The organisations that are performing best share a few common practices.
- They treat patient enquiries as a measurable pipeline rather than a marketing output.
- They align marketing, front-desk teams, and leadership around a single definition of success.
- They prioritise tracking clarity before increasing budgets.
- And most importantly, they use AI and automation to reduce operational burden, without compromising human connection.
In 2026, patient acquisition would be all about running campaigns. It is about building a clean, integrated system that captures intent, qualifies it accurately, responds quickly, and converts it into booked appointments.
Conclusion
If your hospital is running strong campaigns but patient enquiries remain inconsistent, the answer is rarely “we need more ads.” More often, the issue lies within the system.
Growth becomes predictable only when tracking, qualification, and follow-up processes are clear and aligned. As highlighted throughout this article, AI and automation deliver results only when the underlying system is clean and disciplined.
If you are ready to identify where your hospital may be losing potential patients, the Healthcare Marketing Growth Audit provides a simple starting point. For leaders seeking deeper clarity, a follow-up discussion can be requested after completing the audit.
If you share your hospital website and top two specialties, we can often identify initial leakage areas within a single discussion.








